List of primary immunodeficiencies
This is a list of primary immunodeficiencies (PID), which are immune deficiencies that are not secondary to another condition.
The International Union of Immunological Societies recognizes nine classes of primary immunodeficiencies, totaling over 120 conditions. A 2014 update of the classification guide added a 9th category and added 30 new gene defects from the prior 2009 version.[1][2] As of 2018, more than 300 forms of PID have been identified.[3]
Combined T and B–cell immunodeficiencies
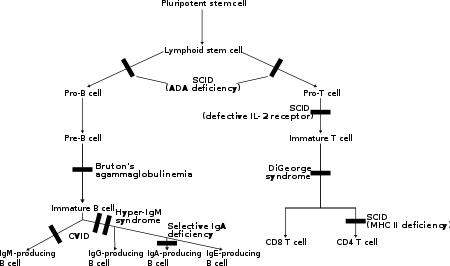
In these disorders both T lymphocytes and often B lymphocytes, regulators of adaptive immunity, are dysfunctional or decreased in number. The main members are various types of severe combined immunodeficiency (SCID).[4]
- T-/B+ SCID (T cells predominantly absent):
- γc deficiency
- JAK3 deficiency
- interleukin 7 receptor chain α deficiency
- CD45 deficiency
- CD3δ, CD3ε, or CD3ζ deficiency
- Coronin-1A deficiency
- T-/B- SCID (both T and B cells absent)
- RAG 1/2 deficiency
- DCLRE1C deficiency
- DNA PKcs deficiency
- adenosine deaminase (ADA) deficiency
- reticular dysgenesis
- Omenn syndrome
- DNA ligase type IV deficiency
- Cernunnos deficiency
- CD40 ligand deficiency
- CD40 deficiency
- Purine nucleoside phosphorylase (PNP) deficiency
- CD3γ deficiency
- CD8 deficiency
- ZAP70 deficiency
- Ca++ channel deficiency
- MHC class I deficiency
- MHC class II deficiency
- Winged helix deficiency
- CD25 deficiency
- CD27 deficiency
- STAT5b deficiency
- ITK deficiency
- SH2D1A deficiency (XLP1)
- MAGT1 deficiency
- DOCK8 deficiency
- RhoH deficiency
- Activated PI3K delta syndrome
- MALT1 deficiency
- BCL10 deficiency
- CARD11 deficiency
- MST1 deficiency
- TCRα deficiency
- LCK deficiency
- IL-21R deficiency
- UNC119 deficiency
- CARD11 deficiency
- OX40 deficiency
- IKBKB deficiency
- Cartilage hair hypoplasia
- LRBA deficiency
Predominantly antibody deficiencies
In primary antibody deficiencies, one or more isotypes of immunoglobulin are decreased or don't function properly. These proteins, generated by plasma cells, normally bind to pathogens, targeting them for destruction.[4]
- Absent B cells with a resultant severe reduction of all types of antibody: X-linked agammaglobulinemia (btk deficiency, or Bruton's agammaglobulinemia), μ-Heavy chain deficiency, l 5 deficiency, Igα deficiency, BLNK deficiency, thymoma with immunodeficiency
- B cells low but present or normal, but with reduction in 2 or more isotypes (usually IgG & IgA, sometimes IgM): common variable immunodeficiency (CVID), ICOS deficiency, CD19 deficiency, TACI (TNFRSF13B) deficiency, BAFF receptor deficiency.
- Normal numbers of B cells with decreased IgG and IgA and increased IgM: Hyper-IgM syndromes
- Normal numbers of B cells with isotype or light chain deficiencies: heavy chain deletions, kappa chain deficiency, isolated IgG subclass deficiency, IgA with IgG subclass deficiency, selective immunoglobulin A deficiency
- Specific antibody deficiency to specific antigens with normal B cell and normal Ig concentrations
- Transient hypogammaglobulinemia of infancy (THI)
Other well defined immunodeficiency syndrome
A number of syndromes escape formal classification but are otherwise recognisable by particular clinical or immunological features.[4]
- Wiskott–Aldrich syndrome
- WIP deficiency
- DNA repair defects not causing isolated SCID:
- Ataxia-telangiectasia
- Ataxia-like syndrome
- Nijmegen breakage syndrome
- Bloom syndrome
- Immunodeficiency–centromeric instability–facial anomalies syndrome (ICF)
- PMS2 deficiency
- RNF168 deficiency
- MCM4 deficiency
- DiGeorge syndrome (when associated with thymic defects)
- CHARGE syndrome
- Immuno-osseous dysplasias (abnormal development of the skeleton with immune problems):
- cartilage–hair hypoplasia
- Schimke syndrome
- Job syndrome
- Tyk2 deficiency
- DOCK8 deficiency
- AR-DKC (autosomal dominant dyskeratosis congenital)
- Hermansky–Pudlak syndrome type 2
- Hyper-IgE syndrome
- Chronic mucocutaneous candidiasis
- Hepatic venoocclusive disease with immunodeficiency (VODI)
- XL-dyskeratosis congenita (Hoyeraal-Hreidarsson syndrome)
- MTHFD1 deficiency
- Comel–Netherton syndrome
- STIM1 deficiency
- STAT5b deficiency
- IKAROS deficiency
- FILS syndrome
Diseases of immune dysregulation
In certain conditions, the regulation rather than the intrinsic activity of parts of the immune system is the predominant problem.[4]
- Immunodeficiency with hypopigmentation or albinism: Chédiak–Higashi syndrome, Griscelli syndrome type 2
- Familial hemophagocytic lymphohistiocytosis: perforin deficiency, UNC13D deficiency, syntaxin 11 deficiency
- X-linked lymphoproliferative syndrome
- Syndromes with autoimmunity:
- (a) Autoimmune lymphoproliferative syndrome: type 1a (CD95 defects), type 1b (Fas ligand defects), type 2a (CASP10 defects), type 2b (CASP8 defects)
- (b) APECED (autoimmune polyendocrinopathy with candidiasis and ectodermal dystrophy)
- (c) IPEX (immunodysregulation polyendocrinopathy enteropathy X-linked syndrome)
- (d) CD25 deficiency
Congenital defects of phagocyte number, function, or both
Phagocytes are the cells that engulf and ingest pathogens (phagocytosis), and destroy them with chemicals. Monocytes/macrophages as well as granulocytes are capable of this process. In certain conditions, either the number of phagocytes is reduced or their functional capacity is impaired.[4]
- Severe Congenital Neutropenia: due to ELA2 deficiency (with myelodysplasia)
- Severe Congenital Neutropenia: due to GFI1 deficiency (with T/B lymphopenia)
- Kostmann syndrome
- Neutropenia with cardiac and urogenital malformations
- Glycogen storage disease type 1b
- Cyclic neutropenia
- X-linked neutropenia/myelodysplasia
- P14 deficiency
- Leukocyte adhesion deficiency type 1
- Leukocyte adhesion deficiency type 2
- Leukocyte adhesion deficiency type 3
- RAC2 deficiency (Neutrophil immunodeficiency syndrome)
- Beta-actin deficiency
- Localized juvenile periodontitis
- Papillon–Lefèvre syndrome
- Specific granule deficiency
- Shwachman–Diamond syndrome
- Chronic granulomatous disease: X-linked
- Chronic granulomatous disease: autosomal (CYBA)
- Chronic granulomatous disease: autosomal (NCF1)
- Chronic granulomatous disease: autosomal (NCF2)
- IL-12 and IL-23 β1 chain deficiency
- IL-12p40 deficiency
- Interferon γ receptor 1 deficiency
- Interferon γ receptor 2 deficiency
- STAT1 deficiency (2 forms)
- AD hyper-IgE
- AR hyper-IgE
- Pulmonary alveolar proteinosis
Defects in innate immunity
Several rare conditions are due to defects in the innate immune system, which is a basic line of defence that is independent of the more advanced lymphocyte-related systems. Many of these conditions are associated with skin problems.[4]
- Hypohidrotic ectodermal dysplasia
- EDA-ID
- IRAK-4 deficiency
- MyD88 deficiency
- WHIM syndrome (warts, hypogammaglobulinaemia, infections, myleokathexis)
- Epidermodysplasia verruciformis
- Herpes simplex encephalitis
- Chronic mucocutaneous candidiasis
- Trypanosomiasis
Autoinflammatory disorder
Rather than predisposing for infections, most of the autoinflammatory disorders lead to excessive inflammation. Many manifest themselves as periodic fever syndromes. They may involve various organs directly, as well as predisposing for long-term damage (e.g. by leading to amyloid deposition).[4]
- Familial Mediterranean fever
- TNF receptor associated periodic syndrome (TRAPS)
- Hyper-IgD syndrome (HIDS)
- CIAS1-related diseases:
- PAPA syndrome (pyogenic sterile arthritis, pyoderma gangrenosum, acne)
- Blau syndrome
- Chronic recurrent multifocal osteomyelitis and congenital dyserythropoietic anemia (Majeed syndrome)
- DIRA (deficiency of the IL-1 receptor antagonist)
Complement deficiencies
The complement system is part of the innate as well as the adaptive immune system; it is a group of circulating proteins that can bind pathogens and form a membrane attack complex. Complement deficiencies are the result of a lack of any of these proteins. They may predispose to infections but also to autoimmune conditions.[4]
- C1q deficiency (lupus-like syndrome, rheumatoid disease, infections)
- C1r deficiency (idem)
- C1s deficiency
- C4 deficiency (lupus-like syndrome)
- C2 deficiency (lupus-like syndrome, vasculitis, polymyositis, pyogenic infections)
- C3 deficiency (recurrent pyogenic infections)
- C5 deficiency (Neisserial infections, SLE)
- C6 deficiency (idem)
- C7 deficiency (idem, vasculitis)
- C8a deficiency
- C8b deficiency
- C9 deficiency (Neisserial infections)
- C1-inhibitor deficiency (hereditary angioedema)
- Factor I deficiency (pyogenic infections)
- Factor H deficiency (haemolytic-uraemic syndrome, membranoproliferative glomerulonephritis)
- Factor D deficiency (Neisserial infections)
- Properdin deficiency (Neisserial infections)
- MBP deficiency (pyogenic infections)
- MASP2 deficiency
- Complement receptor 3 (CR3) deficiency
- Membrane cofactor protein (CD46) deficiency
- Membrane attack complex inhibitor (CD59) deficiency
- Paroxysmal nocturnal hemoglobinuria
- Immunodeficiency associated with ficolin 3 deficiency
Phenocopies of primary immune deficiencies
These are a few specialized autoimmune disorders resulting from environmental rather than genetic causes, which mimic the genotypic disorders.
References
- ↑ Waleed Al-Herz; Aziz Bousfiha; Jean-Laurent Casanova; et al. (2014). "Primary immunodeficiency diseases: an update on the classification from the International Union of Immunological Societies Expert Committee for Primary Immunodeficiency" (PDF). Frontiers in Immunology. 5 (162): 1–33. doi:10.3389/fimmu.2014.00162.
- ↑ Notarangelo L, Casanova JL, Conley ME, et al. (2006). "Primary immunodeficiency diseases: an update from the International Union of Immunological Societies Primary Immunodeficiency Diseases Classification Committee Meeting in Budapest, 2005". J. Allergy Clin. Immunol. 117 (4): 883–96. doi:10.1016/j.jaci.2005.12.1347. PMID 16680902.
- ↑ "Primary Immunodeficiency Disease". Retrieved 30 July 2018.
- 1 2 3 4 5 6 7 8 Notarangelo LD, Fischer A, Geha RS, et al. (December 2009). "Primary immunodeficiencies: 2009 update: The International Union of Immunological Societies (IUIS) Primary Immunodeficiencies (PID) Expert Committee". J. Allergy Clin. Immunol. 124 (6): 1161–78. doi:10.1016/j.jaci.2009.10.013. PMC 2797319. PMID 20004777.