Demodicosis
| Demodicosis | |
|---|---|
 | |
| A dog with severe demodectic mange | |
| Classification and external resources | |
| Specialty | infectious disease |
| ICD-10 | B88.0 (ILDS B88.020) |
| ICD-9-CM | 133.8 |
| DiseasesDB | 33039 |
| eMedicine | article/1203895 |
Demodicosis, also called demodectic mange or red mange, is caused by a sensitivity to and overpopulation of Demodex canis as the hosts immune system is unable to keep the mites under control.
Demodex is a genus of mite in the family Demodicidae. Demodex canis occurs naturally in the hair follicles of most dogs in low numbers around the face and other areas of the body. In most dogs, these mites never cause problems. However, in certain situations, such as an underdeveloped or impaired immune system, intense stress, or malnutrition, the mites can reproduce rapidly, causing symptoms in sensitive dogs that range from mild irritation and hair loss on a small patch of skin to severe and widespread inflammation, secondary infection, and in rare cases can be a life-threatening condition. Small patches of demodicosis often correct themselves over time as the dog's immune system matures, although treatment is usually recommended.
Presentation
Dogs
Minor cases of demodectic mange usually do not cause much itching but might cause pustules on the dog's skin, redness, scaling, leathery, hair loss, warm to the touch, or any combination of these. It most commonly appears first on the face, around the eyes, or at the corners of the mouth, and on the forelimbs and paws. May be misdiagnosed as a "hot spot" or other skin ailment.
In the more severe form, hair loss can occur in patches all over the body and might be accompanied by crusting, pain, enlarged lymph nodes, and deep skin infections.
Demodectic mange is transmitted from host to host through direct contact. Typically animals become infected through nursing from their mother. Demodex mites are host-adapted; there is no zoonotic potential in either canine or feline demodicosis.[1] These mites (Demodex canis) thrive only on their specific hosts (dogs). The transmission of these mites from mother to pup is normal (which is why the mites are normal inhabitants of the dog's skin), but some individuals are sensitive to the mites due to a cellular immune deficiency, underlying disease, stress, or malnutrition,[1] which can lead to the development of clinical demodectic mange.
Some breeds appear to have an increased risk of mild cases as young dogs, including the Afghan Hound, American Staffordshire Terrier, Boston Terrier, Boxer, Chihuahua, Chow Chow, Shar Pei, Collie, Dalmatian, Doberman Pinscher, Bulldog, French Bulldog, English Bull Terrier, Miniature Bull Terrier, German Shepherd Dog, Great Dane, Old English Sheepdog, American Pit Bull Terrier, West Highland White Terrier, Rat Terrier, Yorkshire Terrier, dachshund and Pug.
Humans
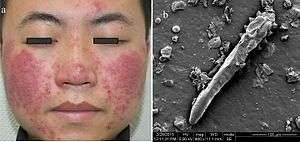
This disease in humans is usually caused by Demodex folliculorum (not the same species affecting dogs) and is usually called demodicosis which may have a rosacea-like appearance.[3][4] Common symptoms include hair loss, itching and inflammation. An association with pityriasis folliculorum has also been described.[4]
Demodicosis is most often seen in folliculitis (inflammation of the hair follicles of the skin). Depending on the location it may result in small pustules (pimples or pustules) at the exit of hair, on inflamed, congested skin. Demodicosis is accompanied by itching, swelling and erythema of the eyelid margins, and the appearance of scales at the base of the eyelashes. Typically, patients complain of eyestrain.
Other
Demodectic mange also occurs in other domestic and wild animals including captive pandas and in China. The mites are specific to their hosts, and each mammal species is host to one or two unique species of Demodex mites. There are two types of demodectic mange in cats. Demodex cati causes follicular mange, similar to that seen in dogs, though it is much less common. Demodex gatoi is a more superficial form of mange, causes an itchy skin condition, and is contagious amongst cats.
Treatment
Localized demodectic mange is considered a common puppyhood ailment, with roughly 90% of cases resolving on their own with no treatment. Minor, localized cases should be left to resolve on their own to prevent masking of the more severe generalized form. If treatment is deemed necessary Goodwinol, a rotenone-based insecticide ointment is often prescribed, but it can be irritating to the skin. Demodectic mange with secondary infection is treated with antibiotics and medicated shampoos.
In more severe generalized cases, Amitraz is a parasiticidal dip that is licensed for use in many countries (the only FDA approved treatment in the USA) for treating canine demodicosis. It is applied weekly or biweekly, for several weeks, until no mites can be detected by skin scrapings. Demodectic mange in dogs can also be managed with avermectins, although there are few countries which license these drugs, which are given by mouth, daily, for this use. Ivermectin is used most frequently; collie-like herding breeds often do not tolerate this drug due to a defect in the blood–brain barrier, though not all of them have this defect. Other avermectin drugs that can be used include doramectin and milbemycin.
Recent results suggest that the isoxazolines afoxolaner and fluralaner, given orally, are effective in treating dogs with generalised demodicosis.[5][6]
Cats with Demodex gatoi must be treated with weekly or bi-weekly sulfurated lime rinses. Demodex cati are treated similarly to canine demodicosis. With veterinary guidance, localized demodectic mange can also be treated with a topical keratolytic and antibacterial agent, followed by a lime sulfur drip or a local application of Rotenone. Ivermectin may also be used. Generalized demodectic mange in cats is more difficult to treat. There are shampoos available that can help to clear dead skin, kill mites and treat bacterial infections. Treatment is in most cases prolonged with multiple applications.[7]
Because of the possibility of the immune deficiency being an inherited trait, many veterinarians believe that all puppies with generalized demodex should be spayed or neutered and not reproduce. Females with generalized demodex should be spayed because the stress of the estrus cycle will often bring on a fresh wave of clinical signs.
Diagnosis
For demodectic mange, properly performed deep skin scrapings generally allow the veterinarian to identify the microscopic mites. Acetate tape impression with squeezing has recently found to be a more sensitive method to identify mites. It was originally thought that because the mite is a normal inhabitant of the dog's skin, the presence of the mites does not conclusively mean the dog suffers from demodex. Recent research, however, found that demodex mite can hardly be found on clinically normal dogs, meaning that the presence of any number of mites in a sample is very likely to be significant. In breeds such as the West Highland White Terrier, relatively minor skin irritation which would otherwise be considered allergy should be carefully scraped because of the predilection of these dogs to demodectic mange. Skin scrapings may be used to follow the progress of treatment in demodectic mange.
Alternatively, plasma levels of zinc and copper have been seen to be decreased in dogs suffering with demodicosis.[8] This may be due to inflammation involved in the immune response of demodicosis which can lead to oxidative stress resulting in dogs suffering from demodicosis to exhibit higher levels of antioxidant productivity.[8] The catalases involved in the antioxidant pathway require the trace minerals zinc and copper. Dogs with demodicosis show a decrease in plasma copper and zinc levels due to the increased demand for antioxidant activity.[8] Therefore, this may be considered as a potential marker for demodicosis.[8]
References
- 1 2 Ectoparasites - Demodex (Mange Mite) Companion Animal Parasite Control (March 2013).
- ↑ Ran Yuping (2016). "Observation of Fungi, Bacteria, and Parasites in Clinical Skin Samples Using Scanning Electron Microscopy". In Janecek, Milos; Kral, Robert. Modern Electron Microscopy in Physical and Life Sciences. InTech. doi:10.5772/61850. ISBN 978-953-51-2252-4.
- ↑ Baima, B.; Sticherling, M. (2002). "Demodicidosis Revisited". Acta Dermato-Venereologica. 82 (1): 3–6. doi:10.1080/000155502753600795. PMID 12013194.
- 1 2 Hsu, Chao-Kai; Hsu, Mark Ming-Long; Lee, Julia Yu-Yun (2009). "Demodicosis: A clinicopathological study". Journal of the American Academy of Dermatology. 60 (3): 453–62. doi:10.1016/j.jaad.2008.10.058. PMID 19231642.
- ↑ Beugnet, Frédéric; Halos, Lénaïg; Larsen, Diane; de Vos, Christa (2016). "Efficacy of oral afoxolaner for the treatment of canine generalised demodicosis". Parasite. 23: 14. doi:10.1051/parasite/2016014. ISSN 1776-1042. PMC 4807374. PMID 27012161.

- ↑ Fourie, Josephus; Liebenberg, Julian; Horak, Ivan; Taenzler, Janina; Heckeroth, Anja; Frénais, Regis (2015). "Efficacy of orally administered fluralaner (BravectoTM) or topically applied imidacloprid/moxidectin (Advocate®) against generalized demodicosis in dogs". Parasites & Vectors. 8: 187. doi:10.1186/s13071-015-0775-8. PMC 4394402. PMID 25881320. Retrieved 20 June 2017.

- ↑ Eldredge, Debra M.; Carlson, Delbert G.; Carlson, Liisa D.; Giffin, James M. (2008). Cat Owner's Veterinary Handbook. Howell Book House. p. 144.
- 1 2 3 4 Dimri, Umesh; Ranjan, R.; Kumar, N.; Sharma, M. C.; Swarup, D.; Sharma, B.; Kataria, M. (2008-06-14). "Changes in oxidative stress indices, zinc and copper concentrations in blood in canine demodicosis". Veterinary Parasitology. 154 (1–2): 98–102. doi:10.1016/j.vetpar.2008.03.001. ISSN 0304-4017. PMID 18440148.
External links
| Wikimedia Commons has media related to dog skin disorders. |