Generalized anxiety disorder
Generalized anxiety disorder (GAD) is an anxiety disorder characterized by excessive, uncontrollable and often irrational worry about events or activities.[4] This excessive worry often interferes with daily functioning, and sufferers are overly concerned about everyday matters such as health issues, money, death, family problems, friendship problems, interpersonal relationship problems, or work difficulties.[5][6] Symptoms may include excessive worry, restlessness, trouble sleeping, feeling tired, irritability, sweating, and trembling.[1]
| Generalized anxiety disorder | |
|---|---|
| Specialty | Psychiatry |
| Symptoms | Excessive worry, restlessness, trouble sleeping, feeling tired, irritability, sweating, trembling[1] |
| Complications | Depression, heart disease, suicide[2] |
| Treatment | Behavioral therapy, medications |
| Frequency | 3–5% (lifetime prevalence)[3] |
These symptoms must be consistent and ongoing, persisting at least six months, for a formal diagnosis of GAD.[4][5] GAD is also common in individuals with a history of substance abuse and a family history of the disorder.[7] Standardized rating scales such as GAD-7 can be used to assess severity of GAD symptoms.[8]
Medications which have been found to be useful include duloxetine, pregabalin, venlafaxine, and escitalopram.[9]
In a given year, about two percent of American adults and European adults experience GAD.[10][11] Globally about 4% are affected at some point in their life.[3] GAD is seen in women twice as frequently as men.[12]
Risk factors
Genetics
Genes are attributed to about a third of general anxiety disorder's variance.[13] Individuals with a genetic predisposition for GAD are more likely to develop GAD, especially in response to a life stressor.[14]
Substance-induced
Long-term use of benzodiazepines can worsen underlying anxiety,[15][16] with evidence that reduction of benzodiazepines can lead to a diminishment of anxiety symptoms.[17] Similarly, long-term effects of alcohol consumption is associated with anxiety disorders,[18] with evidence that prolonged abstinence can result in a disappearance of anxiety symptoms.[19] However, it can take up to two years for anxiety symptoms to return to baseline in about a quarter of people recovering from alcoholism.[20]
In one study in 1988–90, illness in approximately half of patients attending mental health services at British hospital psychiatric clinics, for conditions such as panic disorder or social phobia, was determined to be the result of alcohol or benzodiazepine dependence. In these patients, anxiety symptoms, while worsening initially during the withdrawal phase, disappeared with abstinence from benzodiazepines or alcohol. Sometimes anxiety pre-existed alcohol or benzodiazepine dependence, but the dependence was acting to keep the anxiety disorders going and could progressively make them worse. Recovery from benzodiazepines tends to take a lot longer than recovery from alcohol, but people can regain their previous good health.[20]
Tobacco smoking has been established as a risk factor for developing anxiety disorders.[21] Neurotransmitter systems, inflammation, oxidative stress, mitochondria dysfunction and neurogenesis are affected by exposure to cigarette smoke which are all pathways thought to be associated with GAD.[22]
Excessive caffeine use has also been linked to aggravating and maintaining anxiety.[23] This is due to overactivation of the sympathetic nervous system.[24]
Other
Populations with a higher rate of diagnosis of GAD include individuals with low and middle socio-economic status and those who are separated, divorced, unemployed, widowed or have low levels of education.[25]
African Americans have higher odds of having GAD and the disorder often manifests itself in different patterns.[26][27]
GAD is also common in the elderly population.[28]
Low self-esteem, disrupted family environments and sexual abuse also increase the risk of GAD.
Pathophysiology
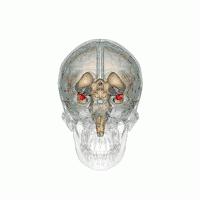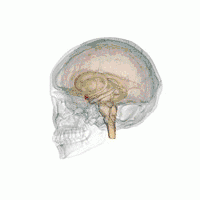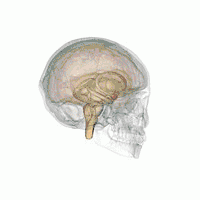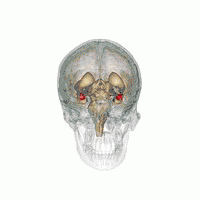
Generalized anxiety disorder has been linked to disrupted functional connectivity of the amygdala and its processing of fear and anxiety.[29] Sensory information enters the amygdala through the nuclei of the basolateral complex (consisting of lateral, basal and accessory basal nuclei). The basolateral complex processes the sensory-related fear memories and communicates their threat importance to memory and sensory processing elsewhere in the brain, such as the medial prefrontal cortex and sensory cortices.
Another area, the adjacent central nucleus of the amygdala, controls species-specific fear responses in its connections to the brainstem, hypothalamus and cerebellum areas. In those with generalized anxiety disorder, these connections seem less functionally distinct, and there is greater gray matter in the central nucleus. Another difference is that the amygdala areas have decreased connectivity with the insula and cingulate areas that control general stimulus salience, while having greater connectivity with the parietal cortex and prefrontal cortex circuits that underlie executive functions.[29] The latter suggests a compensation strategy for dysfunctional amygdala processing of anxiety. This is consistent with cognitive theories that suggest the use in this disorder of attempts to reduce the involvement of emotions with compensatory cognitive strategies.[29]
Diagnosis
DSM-5 criteria
The diagnostic criteria for GAD as defined by the Diagnostic and Statistical Manual of Mental Disorders DSM-5 (2013),[4] published by the American Psychiatric Association, are paraphrased as follows:[4]
- Too much anxiety or worry over more than six months. This is present most of the time in regards to many activities.
- Inability to manage these symptoms
- At least three of the following occur:
Note: Only one item is required in children.- Restlessness
- Tires easily
- Problems concentrating
- Irritability
- Muscle tension.
- Problems with sleep
- Symptoms result in problems with functioning.
- Symptoms are not due to medications, drugs, other physical health problems
- Symptoms do not fit better with another psychiatric problem such as panic disorder
No major changes to GAD have occurred since publication of the Diagnostic and Statistical Manual of Mental Disorders (2004); minor changes include wording of diagnostic criteria.[30]
ICD-10 criteria
ICD-10 Generalized anxiety disorder "F41.1"[31] Note: For children different criteria may be applied (see F93.80).
- A period of at least six months with prominent tension, worry, and feelings of apprehension, about everyday events and problems.
- At least four symptoms out of the following list of items must be present, of which at least one from items (1) to (4).
- Autonomic arousal symptoms
- (1) Palpitations or pounding heart, or accelerated heart rate.
- (2) Sweating.
- (3) Trembling or shaking.
- (4) Dry mouth (not due to medication or dehydration).
- Symptoms concerning chest and abdomen
- (5) Difficulty breathing.
- (6) Feeling of choking.
- (7) Chest pain or discomfort.
- (8) Nausea or abdominal distress (e.g. churning in the stomach).
- Symptoms concerning brain and mind
- (9) Feeling dizzy, unsteady, faint or light-headed.
- (10) Feelings that objects are unreal (derealization), or that one's self is distant or "not really here" (depersonalization).
- (11) Fear of losing control, going crazy, or passing out.
- (12) Fear of dying.
- General symptoms
- (13) Hot flashes or cold chills.
- (14) Numbness or tingling sensations.
- Symptoms of tension
- (15) Muscle tension or aches and pains.
- (16) Restlessness and inability to relax.
- (17) Feeling keyed up, or on edge, or of mental tension.
- (18) A sensation of a lump in the throat or difficulty with swallowing.
- Other non-specific symptoms
- (19) Exaggerated response to minor surprises or being startled.
- (20) Difficulty in concentrating or mind going blank, because of worrying or anxiety.
- (21) Persistent irritability.
- (22) Difficulty getting to sleep because of worrying.
- The disorder does not meet the criteria for panic disorder (F41.0), phobic anxiety disorders (F40.-), obsessive-compulsive disorder (F42.-) or hypochondriacal disorder (F45.2).
- Most commonly used exclusion criteria: not sustained by a physical disorder, such as hyperthyroidism, an organic mental disorder (F0) or psychoactive substance-related disorder (F1), such as excess consumption of amphetamine-like substances, or withdrawal from benzodiazepines.[32]
Prevention
Increased core temperature can help to relax muscles.[33]
Foods high in omega-3 fatty acids including oily fish such as salmon and mackerel reduce the inflammatory response and thus increase serotonin availability.[34]
Many people have found ease through relaxation exercises, deep breathing practice, and meditation.[35]
Additionally, avoidance of caffeine may prevent GAD.[36]
Avoiding nicotine also can decrease the risk for the development of anxiety disorders including generalized anxiety disorder.[37]
Treatment
Once GAD develops, it is possible for it to become chronic, but can be managed or eliminated with proper treatment.[38]
Both cognitive behavioral therapy (CBT) and medications (such as SSRIs) have been shown to be effective in reducing anxiety. A comparison of overall outcomes of CBT and medication on anxiety did not show statistically significant differences (i.e. they were equally effective in treating anxiety). However, CBT is significantly more effective in reducing depression severity, and its effects are more likely to be maintained in the long term, whereas the effectiveness of pharmacologic treatment tends to lessen if medication is discontinued.[39] A combination of both CBT and medication is generally seen as the most desirable approach to treatment.[40] Use of medication to lower extreme anxiety levels can be important in enabling patients to engage effectively in CBT.
Lifestyle
Lifestyle factors including: stress management, stress reduction, relaxation, exercise, sleep hygiene, caffeine, and alcohol can influence the persistence of anxiety. Stress is a factor that can trigger anxiety. Therefore, keeping stress levels low through stress management, stress reduction, and relaxation may be beneficial. Physical activity has shown to have a positive impact whereas low physical activity may be a risk factor for anxiety disorders.[41]
Therapy
Generalized anxiety disorder is based on psychological components that include cognitive avoidance, positive worry beliefs, ineffective problem-solving and emotional processing, interpersonal issues, previous trauma, intolerance of uncertainty, negative problem orientation, ineffective coping, emotional hyperarousal, poor understanding of emotions, negative cognitive reactions to emotions, maladaptive emotion management and regulation, experiential avoidance, and behavioral restriction.[42] To combat the previous cognitive and emotional aspects of GAD, psychologists often include some of the following key treatment components in their intervention plan; self-monitoring, relaxation techniques, self-control desensitization, gradual stimulus control, cognitive restructuring, worry outcome monitoring, present-moment focus, expectancy-free living, problem-solving techniques, processing of core fears, socialization, discussion and reframing of worry beliefs, emotional skills training, experiential exposure, psychoeducation, mindfulness and acceptance exercises.[42] There exist behavioral, cognitive, and a combination of both treatments for GAD that focus on some of those key components.
Among the cognitive–behavioral orientated psychotherapies the two main treatments are cognitive behavioral therapy and acceptance and commitment therapy (ACT).[43] Intolerance of uncertainty therapy and motivational interviewing are two new treatments for GAD that are used as either stand-alone treatments or additional strategies that may enhance CBT.[44]
Cognitive behavioral therapy
Cognitive behavioral therapy (CBT) appears to be useful in the treatment of generalized anxiety disorder.[45] However, there is still room for improvement because only about 50% of those who complete treatments achieve higher functioning or recovery after treatment. Therefore, there's a need for enhancement of current components of CBT.[44] CBT usually helps one-third of the patients substantially, whilst another third does not respond at all to treatment.[46]
CBT is a psychological method of treatment that involves a therapist working with the person to understand how thoughts and feelings influence behaviour.[47] Elements of the therapy include exposure strategies to allow the patient to confront their anxieties gradually and feel more comfortable in anxiety-provoking situations, as well as to practice the skills they have learned. CBT can be used alone or in conjunction with medication.[48]
Albert Ellis is one such notable cognitive theorist, and practitioner who coined the term "maladaptive assumptions."[49] These maladaptive assumptions, negatively incorporated in a client's thought patterns, may serve to disrupt the ability to engage in healthy interactions.[49] Frequent use of such maladaptive assumption such as, "It is awful and catastrophic when things are not the way one would very much like them to be" may provoke further anxiety over the course of events.[49] Thus rational-emotive therapy, a form of cognitive behavioral therapy, may be implemented to counter clients' maladaptive assumptions, and educate them about the part excessive worrying plays in resulting cognitive interpretations across a span of social situations.
Components of CBT for GAD includes psychoeducation, self-monitoring, stimulus control techniques, relaxation, self-control desensitization, cognitive restructuring, worry exposure, worry behavior modification, and problem-solving. The first step in the treatment of GAD is informing of the patient about the issues and the plan of the solution. The purpose of psychoeducation is to provide some relief, destigmatization of the disorder, motivating, and accomplishing participation by making the patient understand the program of treatment. The purpose of this component is to identify cues that provoke the anxiety. Stimulus control intervention refers to minimizing the stimulus conditions under which worrying occurs. Relaxation techniques lower the patients' stress and thus increase attention to alternatives in feared situations (other than worrying). Deep breathing exercise, progressive muscle relaxation, and applied relaxation fall under the scope of relaxation techniques.[44]
Self-control desensitization involves patients being deeply relaxed before vividly imagining themselves in situations that usually make them anxious and worry until internal anxiety cues are triggered. Patients then imagine themselves coping with the situation and decreasing their anxious response. If anxiety diminishes, they then enter a deeper relaxed state and turn off the scene. The purpose of cognitive restructuring is to shift from a worrisome outlook to a more functional and adaptive perception of the world, the future, and the self. It involves Socratic questioning that leads patients to think through their worries and anxieties so they can realize that alternative interpretations and feelings are more accurate. It also involves behavioral experiments that actually test the validity of both the negative and alternative thoughts in real-life situations. In CBT for GAD, patients also engage in worry exposure exercises during which they are asked to imagine themselves exposed to images of the most feared outcomes. Then they engage in response-prevention instruction that prevents them from avoiding the image and motivates alternative outcomes to the feared stimulus. The goals of worry exposure are habituation and reinterpretation of the meaning of the feared stimulus. Worry behavior prevention requires patients to monitor the behaviors that caused them worry and are then asked to prevent themselves from engaging in them. Instead, they are encouraged to use other coping mechanisms learned earlier in the treatment. Finally, problem solving focuses on dealing with current problems through a problem-solving approach: (1) definition of the problem, (2) formulation of goals, (3) creation of alternative solutions, (4) decision-making, and (5) implementing and verifying the solutions.[44]
Acceptance and commitment therapy
Acceptance and commitment therapy (ACT) is a behavioral treatment based on acceptance-based models. ACT is designed with the purpose to target three therapeutic goals: (1) reduce the use of avoiding strategies intended to avoid feelings, thoughts, memories, and sensations; (2) decreasing a person's literal response to their thoughts (e.g., understanding that thinking "I'm hopeless" does not mean that the person's life is truly hopeless), and (3) increasing the person's ability to keep commitments to changing their behaviors. These goals are attained by switching the person's attempt to control events to working towards changing their behavior and focusing on valued directions and goals in their lives as well as committing to behaviors that help the individual accomplish those personal goals.[50] This psychological therapy teaches mindfulness (paying attention on purpose, in the present, and in a nonjudgmental manner) and acceptance (openness and willingness to sustain contact) skills for responding to uncontrollable events and therefore manifesting behaviors that enact personal values.[51] Like many other psychological therapies, ACT works best in combination with pharmacology treatments.
Intolerance of uncertainty therapy
Intolerance of uncertainty therapy (IUT) refers to a consistent negative reaction to uncertain and ambiguous events regardless of their likelihood of occurrence. IUT is used as a stand-alone treatment for GAD patients. Thus, IUT focuses on helping patients in developing the ability to tolerate, cope with and accept uncertainty in their life in order to reduce anxiety. IUT is based on the psychological components of psychoeducation, awareness of worry, problem-solving training, re-evaluation of the usefulness of worry, imagining virtual exposure, recognition of uncertainty, and behavioral exposure. Studies have shown support for the efficacy of this therapy with GAD patients with continued improvements in follow-up periods.[44]
Motivational interviewing
A promising innovative approach to improving recovery rates for the treatment of GAD is to combine CBT with motivational interviewing (MI). Motivational interviewing is a strategy centered on the patient that aims to increase intrinsic motivation and decrease ambivalence about change due to the treatment. MI contains four key elements: (1) express empathy, (2) heighten dissonance between behaviors that are not desired and values that are not consistent with those behaviors, (3) move with resistance rather than direct confrontation, and (4) encourage self-efficacy. It is based on asking open-ended questions and listening carefully and reflectively to patients' answers, eliciting "change talk", and talking with patients about the pros and cons of change. Some studies have shown the combination of CBT with MI to be more effective than CBT alone.[44]
Medications
An international review of psychiatrists' management of patients with generalized anxiety disorder (GAD) reported that the preferred first-line pharmacological treatments of GAD were selective serotonin reuptake inhibitors (SSRIs) (80%), followed by serotonin–norepinephrine reuptake inhibitors (SNRIs) (43%), and pregabalin (35%). Preferred second-line treatments were SNRIs (41%) and pregabalin (36%).[52]
Selective serotonin reuptake inhibitors
Pharmaceutical treatments for GAD include selective serotonin reuptake inhibitors (SSRIs).[48] These are the preferred first line of treatment.[52] These increase serotonin levels through inhibition of serotonin reuptake receptors.[53]
FDA approved SSRIs used for this purpose include escitalopram[54] and paroxetine.[55] However, guidelines suggest using sertraline first due to its cost-effectiveness compared to other SSRIs used for generalized anxiety disorder and a lower risk of withdrawal compared to SNRIs. If sertraline is found to be ineffective, then it is recommended to try another SSRI or SNRI.[56]
Common side effects include nausea, sexual dysfunction, headache, diarrhea, constipation, restlessness, increased risk of suicide in young adults and adolescents,[57] among others. Sexual side effects, weight gain, and higher risk of withdrawal are more common in paroxetine than escitalopram and sertraline.[58] In older populations or those taking concomitant medications that increase risk of bleeding, SSRIs may further increase the risk of bleeding.[56] Overdose of an SSRI or concomitant use with another agent that causes increased levels of serotonin can result in serotonin syndrome, which can be life-threatening.
Serotonin norepinephrine reuptake inhibitors
First line pharmaceutical treatments for GAD also include serotonin-norepinephrine reuptake inhibitors (SNRIs).[59] These inhibit the reuptake of serotonin and noradrenaline to increase their levels in the CNS.[60]
FDA approved SNRIs used for this purpose include duloxetine (Cymbalta) and venlafaxine (Effexor).[61][62] While SNRIs have similar efficacy as SSRIs,[63] many psychiatrists prefer to use SSRIs first in the treatment of Generalized Anxiety Disorder.[61][64][65][66] The slightly higher preference for SSRIs over SNRIs as a first choice for treatment of anxiety disorders may have been influenced by the observation of poorer tolerability of the SNRIs in comparison to SSRIs in systematic reviews of studies of depressed patients.[67][68][69] Duloxetine is also indicated for the treatment of chronic musculoskeletal pain and neuropathic pain associated with diabetes mellitus,[70] and may be a good option for people with both conditions.[66]
Side effects common to both SNRIs include anxiety, restlessness, nausea, weight loss, insomnia, dizziness, drowsiness, sweating, dry mouth, sexual dysfunction and weakness.[71] In comparison to SSRIs, the SNRIs have a higher prevalence of the side effects of insomnia, dry mouth, nausea and high blood pressure.[71][72] Both SNRIs have the potential for discontinuation syndrome after abrupt cessation, which can precipitate symptoms including motor disturbances and anxiety and may require tapering.[70][73] Like other serotonergic agents, SNRIs have the potential to cause serotonin syndrome, a potentially fatal systemic response to serotonergic excess that causes symptoms including agitation, restlessness, confusion, tachycardia, hypertension, mydriasis, ataxia, myoclonus, muscle rigidity, diaphoresis, diarrhea, headache, shivering, goose bumps, high fever, seizures, arrhythmia and unconsciousness.[74] SNRIs like SSRIs carry a black box warning for suicidal ideation, but it is generally considered that the risk of suicide in untreated depression is far higher than the risk of suicide when depression is properly treated.[75]
Benzodiazepines
Benzodiazepines are most often prescribed to people with generalized anxiety disorder. Research suggests that these medications give some relief, at least in the short term. However, they carry some risks, mainly impairment of both cognitive and motor functioning, and psychological and physical dependence that makes it difficult for patients to stop taking them. It has been noted that people taking benzodiazepines are not as alert on their job or at school. Additionally, these medications may impair driving and they are often associated with falls in the elderly, resulting in hip fractures. These shortcomings make the use of benzodiazepines optimal only for short-term relief of anxiety.[76] CBT and medication are of comparable efficacy in the short-term but CBT has advantages over medication in the longer term.[77]
Benzodiazepines (or "benzos") are fast-acting hypnotic sedatives that are also used to treat GAD and other anxiety disorders.[48] Benzodiazepines are prescribed for generalized anxiety disorder and show beneficial effects in the short term. Popular benzodiazepines for GAD include alprazolam, lorazepam, and clonazepam. The World Council of Anxiety does not recommend the long-term use of benzodiazepines because they are associated with the development of tolerance, psychomotor impairment, cognitive and memory impairments, physical dependence and a withdrawal syndrome.[78][79] Side effects include drowsiness, reduced motor coordination and problems with equilibrioception.
Pregabalin and gabapentin
Pregabalin (Lyrica) acts on the voltage-dependent calcium channel to decrease the release of neurotransmitters such as glutamate, norepinephrine and substance P. Its therapeutic effect appears after 1 week of use and is similar in effectiveness to lorazepam, alprazolam and venlafaxine but pregabalin has demonstrated superiority by producing more consistent therapeutic effects for psychic and somatic anxiety symptoms. Long-term trials have shown continued effectiveness without the development of tolerance and additionally, unlike benzodiazepines, it does not disrupt sleep architecture and produces less severe cognitive and psychomotor impairment. It also has a low potential for abuse and dependency and may be preferred over the benzodiazepines for these reasons.[80][81] The anxiolytic effects of pregabalin appear to persist for at least six months continuous use, suggesting tolerance is less of a concern; this gives pregabalin an advantage over certain anxiolytic medications such as benzodiazepines.[82]
Gabapentin (Neurontin), a closely related medication to pregabalin with the same mechanism of action, has also demonstrated effectiveness in the treatment of GAD,[83] though unlike pregabalin, it has not been approved specifically for this indication. Nonetheless, it is likely to be of similar usefulness in the management of this condition, and by virtue of being off-patent, it has the advantage of being significantly less expensive in comparison.[84] In accordance, gabapentin is frequently prescribed off-label to treat GAD.[85]
Other psychiatric medications
- 5-HT1A receptor partial agonists, such as buspirone. Buspirone is an FDA approved first line agent, to be used if SSRI/SNRIs are contraindicated or fail as a treatment. Like the SSRI/SNRIs buspirone has a 2-4 week delayed onset of action and a maximum benefit seen at 4–6 weeks. Common side effects include dizziness, nausea, and headache. This is a well-tolerated drug with no sedation or sexual side effects, which are commonly seen with SSRI/SNRIs. However, buspirone is not as effective in patients who have been previously treated with benzodiazepines.[86]
- Newer, atypical serotonergic antidepressants, such as vilazodone and agomelatine.
- Tricyclic antidepressants (TCAs), such as imipramine and clomipramine.
- Certain monoamine oxidase inhibitors (MAOIs), such as moclobemide and phenelzine.
Other medications
- Hydroxyzine - Antihistamine, 5-HT2A receptor antagonist.
- Propranolol - Sympatholytic, beta blocker.
- Clonidine - Sympatholytic, α2-adrenergic receptor agonist.
- Guanfacine - Sympatholytic, α2-adrenergic receptor agonist.
- Prazosin - Sympatholytic, alpha blocker.
Comorbidity
Depression
In the National Comorbidity Survey (2005), 58 percent of patients diagnosed with major depression were found to have an anxiety disorder; among these patients, the rate of comorbidity with GAD was 17.2 percent, and with panic disorder, 9.9 percent. Patients with a diagnosed anxiety disorder also had high rates of comorbid depression, including 22.4 percent of patients with social phobia, 9.4 percent with agoraphobia, and 2.3 percent with panic disorder. A longitudinal cohort study found 12% of the 972 participants had GAD comorbid with MDD.[87] Accumulating evidence indicates that patients with comorbid depression and anxiety tend to have greater illness severity and a lower treatment response than those with either disorder alone.[88] In addition, social function and quality of life are more greatly impaired.
For many, the symptoms of both depression and anxiety are not severe enough (i.e. are subsyndromal) to justify a primary diagnosis of either major depressive disorder (MDD) or an anxiety disorder. However, dysthymia is the most prevalent comorbid diagnosis of GAD clients. Patients can also be categorized as having mixed anxiety-depressive disorder, and they are at significantly increased risk of developing full-blown depression or anxiety.
Various explanations for the high comorbidity between GAD and depressive disorders have been suggested, including genetic pleiotropy, meaning that GAD and nonbipolar depression might represent different phenotypic expressions of a common etiology.[89]
Substance use disorders
Those with GAD have a lifetime comorbidity prevalence of 30% to 35% with alcohol use disorder and 25% to 30% for another substance use disorder.[90] People with both GAD and a substance use disorder also have a higher lifetime prevalence for other comorbidities.[90] A study found that GAD was the primary disorder in slightly more than half of the 18 participants that were comorbid with alcohol use disorder.[91]
Other comorbidities
GAD often coexists with conditions associated with stress, such as muscle tension and irritable bowel syndrome.[92]
Patients with GAD can sometimes present with symptoms such as insomnia or headaches as well as pain and interpersonal problems.[93]
Further research suggests that about 20 to 40 percent of individuals with attention deficit hyperactivity disorder have comorbid anxiety disorders, with GAD being the most prevalent.[94]
Comorbidity and treatment
Therapy has been shown to have equal efficacy in patents with GAD and patients with GAD and comorbid disorders. Patients with comorbid disorders have more severe symptoms when starting therapy but demonstrated a greater improvement than patients with simple GAD.
Pharmacological approaches i.e. the use of antidepressants must be adapted for different comorbidities. For example, serotonin reuptake inhibitors and short acting benzodiazepines (BZDs) are used for depression and anxiety. However, for patients with anxiety and substance abuse, BZDs should be avoided due to their abuse liability.[95] CBT has been found an effective treatment since it improves symptoms of GAD and substance abuse.
Compared to the general population, patients with internalizing disorders such as depression, generalized anxiety disorder (GAD) and post-traumatic stress disorder (PTSD) have higher mortality rates, but die of the same age-related diseases as the population, such as heart disease, cerebrovascular disease and cancer.[96]
History
The American Psychiatric Association introduced GAD as a diagnosis in the DSM-III in 1980, when anxiety neurosis was split into GAD and panic disorder.[89] The definition in the DSM-III required uncontrollable and diffuse anxiety or worry that is excessive and unrealistic and persists for 1 month or longer. High rates in comorbidity of GAD and major depression led many commentators to suggest that GAD would be better conceptualized as an aspect of major depression instead of an independent disorder.[97] Many critics stated that the diagnostic features of this disorder were not well established until the DSM-III-R.[98] Since comorbidity of GAD and other disorders decreased with time, the DSM-III-R changed the time requirement for a GAD diagnosis to 6 months or longer.[99] The DSM-IV changed the definition of excessive worry and the number of associated psychophysiological symptoms required for a diagnosis.[97] Another aspect of the diagnosis the DSM-IV clarified was what constitutes a symptom as occurring "often".[100] The DSM-IV also required difficulty controlling the worry to be diagnosed with GAD. The DSM-5 emphasized that excessive worrying had to occur more days than not and on a number of different topics.[98] It has been stated that the constant changes in the diagnostic features of the disorder have made assessing epidemiological statistics such as prevalence and incidence difficult, as well as increasing the difficulty for researchers in identifying the biological and psychological underpinnings of the disorder. Consequently, making specialized medications for the disorder is more difficult as well. This has led to the continuation of GAD being medicated heavily with SSRIs.[98]
Epidemiology
4% are affected at some point in their life.[3] GAD is seen in women twice as much as men.[12] It has been suggested that this is primarily because women are more likely than men to live in poverty, be subject to discrimination, and be sexually and physically abused.[101]
USA
GAD is the most common cause of disability in the workplace in the United States.[102]
United States: Approximately 3.1 percent of people age 18 and over in a given year (9.5 million).[10]
UK
5.9 percent of adults were affected by GAD in 2019.[103]
Other
- Australia: 3 percent of adults[104]
- Canada: 2.5 percent[105]
- Italy: 2.9 percent[106]
- Taiwan: 0.4 percent[106]
The usual age of onset is variable, from childhood to late adulthood, with the median age of onset being approximately 31[107] and mean age of onset being 32.7.[108] Most studies find that GAD is associated with an earlier and more gradual onset than the other anxiety disorders.[109] The prevalence of GAD in children is approximately 3%; the prevalence in adolescents is reported as high as 10.8%.[110] When GAD appears in children and adolescents, it typically begins around 8 to 9 years of age.[111]
See also
- Daily Assessment of Symptoms – Anxiety
References
- "Generalized Anxiety Disorder: When Worry Gets Out of Control". NIMH. Retrieved 30 May 2019.
- DeMartini, J; Patel, G; Fancher, TL (2 April 2019). "Generalized Anxiety Disorder". Annals of Internal Medicine. 170 (7): ITC49–ITC64. doi:10.7326/AITC201904020. PMID 30934083.
- Craske, MG; Stein, MB (24 June 2016). "Anxiety". The Lancet. 388 (10063): 3048–3059. doi:10.1016/S0140-6736(16)30381-6. PMID 27349358.
- Diagnostic and statistical manual of mental disorders : DSM-5 (5th ed.). Washington, D.C.: American Psychiatric Association. 2013. p. 222. ISBN 978-0-89042-554-1.
- "What Is Generalized Anxiety Disorder?", National Institute of Mental Health. Accessed 28 May 2008.
- Torpy, Janet M.; Burke, AE; Golub, RM (2011). "Generalized Anxiety Disorder". JAMA. 305 (5): 522. doi:10.1001/jama.305.5.522. PMID 21285432.
- Patel, Gayatri; Fancher, Tonya L (2013). "In The Clinic: Generalized Anxiety Disorder". Annals of Internal Medicine. 159 (11): ITC6–1, ITC6–2, ITC6–3, ITC6–4, ITC6–5, ITC6–6, ITC6–7, ITC6–8, ITC6–9, ITC6–10, ITC6–11, quiz ITC6–12. doi:10.7326/0003-4819-159-11-201312030-01006. PMID 24297210.
- Spitzer, Robert L.; Kroenke, K; Williams, JB; Löwe, B (2006). "A Brief Measure for Assessing Generalized Anxiety Disorder". Archives of Internal Medicine. 166 (10): 1092–7. doi:10.1001/archinte.166.10.1092. PMID 16717171.
- Slee, April; Nazareth, Irwin; Bondaronek, Paulina; Liu, Yifeng; Cheng, Zhihang; Freemantle, Nick (February 2019). "Pharmacological treatments for generalised anxiety disorder: a systematic review and network meta-analysis". The Lancet. 393 (10173): 768–777. doi:10.1016/S0140-6736(18)31793-8. PMID 30712879.
- "The Numbers Count" Archived 2014-07-28 at the Wayback Machine, National Institute of Mental Health. Accessed 28 May 2007.
- Lieb, Roselind; Becker, Eni; Altamura, Carlo (2005). "The epidemiology of generalized anxiety disorder in Europe". European Neuropsychopharmacology. 15 (4): 445–52. doi:10.1016/j.euroneuro.2005.04.010. PMID 15951160.
- Geddes, John; Price, Jonathan; Gelder, Rebecca McKnight; with Michael; Mayou, Richard (2012). Psychiatry (4th ed.). Oxford: Oxford University Press. p. 287. ISBN 9780199233960.
- Hettema, J. M.; Neale, MC; Kendler, KS (2001). "A Review and Meta-Analysis of the Genetic Epidemiology of Anxiety Disorders". American Journal of Psychiatry. 158 (10): 1568–78. doi:10.1176/appi.ajp.158.10.1568. PMID 11578982.
- Donner, Jonas; Pirkola, Sami; Silander, Kaisa; Kananen, Laura; Terwilliger, Joseph D.; Lönnqvist, Jouko; Peltonen, Leena; Hovatta, Iiris (2008). "An Association Analysis of Murine Anxiety Genes in Humans Implicates Novel Candidate Genes for Anxiety Disorders". Biological Psychiatry. 64 (8): 672–80. doi:10.1016/j.biopsych.2008.06.002. PMC 2682432. PMID 18639233.
- Galanter, Marc (1 July 2008). The American Psychiatric Publishing Textbook of Substance Abuse Treatment (American Psychiatric Press Textbook of Substance Abuse Treatment) (4 ed.). American Psychiatric Publishing, Inc. p. 197. ISBN 978-1-58562-276-4.
- Ashton, Heather (2005). "The diagnosis and management of benzodiazepine dependence". Current Opinion in Psychiatry. 18 (3): 249–55. doi:10.1097/01.yco.0000165594.60434.84. PMID 16639148.
- Lindsay, S. J. E.; Powell, Graham E., eds. (28 July 1998). The Handbook of Clinical Adult Psychology (2nd ed.). Routledge. p. 173. ISBN 978-0-415-07215-1.
- Cargiulo, T. (2007). "Understanding the health impact of alcohol dependence". American Journal of Health-System Pharmacy. 64 (5 Supplement 3): S5–11. doi:10.2146/ajhp060647. PMID 17322182.
- Wetterling, T; Junghanns, K (2000). "Psychopathology of alcoholics during withdrawal and early abstinence". European Psychiatry. 15 (8): 483–8. doi:10.1016/S0924-9338(00)00519-8. PMID 11175926.
- Cohen, SI (1995). "Alcohol and benzodiazepines generate anxiety, panic and phobias". Journal of the Royal Society of Medicine. 88 (2): 73–7. PMC 1295099. PMID 7769598.
- Morissette SB, Tull MT, Gulliver SB, Kamholz BW, Zimering RT (March 2007). "Anxiety, anxiety disorders, tobacco use, and nicotine: a critical review of interrelationships". Psychological Bulletin. 133 (2): 245–72. doi:10.1037/0033-2909.133.2.245. PMID 17338599.
- Moylan S, Jacka FN, Pasco JA, Berk M (May 2013). "How cigarette smoking may increase the risk of anxiety symptoms and anxiety disorders: a critical review of biological pathways". Brain and Behavior. 3 (3): 302–26. doi:10.1002/brb3.137. PMC 3683289. PMID 23785661.
- Bruce M. S., Lader M.; Lader (2009). "Caffeine abstention in the management of anxiety disorders". Psychological Medicine. 19 (1): 211–4. doi:10.1017/S003329170001117X. PMID 2727208.
- Jaberi, Neema; Hardwick, Elizabeth; Winston, Anthony P. (November 2005). "Neuropsychiatric effects of caffeine". Advances in Psychiatric Treatment. 11 (6): 432–439. doi:10.1192/apt.11.6.432. ISSN 1472-1481.
- Ansseau, Marc; Fischler, Benjamin; Dierick, Michel; Albert, Adelin; Leyman, Sophie; Mignon, Annick (26 June 2007). "Socioeconomic correlates of generalized anxiety disorder and major depression in primary care: The GADIS II study (Generalized Anxiety and Depression Impact Survey II)". Depression and Anxiety. 25 (6): 506–513. doi:10.1002/da.20306. PMID 17595015.
- Soto, José A.; Dawson-Andoh, Nana A.; Belue, Rhonda (March 2011). "The relationship between perceived discrimination and Generalized Anxiety Disorder among African Americans, Afro Caribbeans, and non-Hispanic Whites". Journal of Anxiety Disorders. 25 (2): 258–265. doi:10.1016/j.janxdis.2010.09.011. PMC 3053120. PMID 21041059.
- Neal, Angela M.; Turner, Samuel M. (May 1991). "Anxiety disorders research with African Americans: Current status". Psychological Bulletin. 109 (3): 400–410. doi:10.1037/0033-2909.109.3.400. PMID 2062979.
- Cameron, Alasdair (2004). Crash Course Psychiatry. Elsevier Ltd. ISBN 978-0-7234-3340-8.
- Etkin, Amit; Prater, Katherine E.; Schatzberg, Alan F.; Menon, Vinod; Greicius, Michael D. (2009). "Disrupted Amygdalar Subregion Functional Connectivity and Evidence of a Compensatory Network in Generalized Anxiety Disorder". Archives of General Psychiatry. 66 (12): 1361–72. doi:10.1001/archgenpsychiatry.2009.104. PMID 19996041.
- Möller, Hans-Jürgen; Bandelow, Borwin; Bauer, Michael; Hampel, Harald; Herpertz, Sabine C.; Soyka, Michael; Barnikol, Utako B.; Lista, Simone; Severus, Emanuel; Maier, Wolfgang (26 August 2014). "DSM-5 reviewed from different angles: goal attainment, rationality, use of evidence, consequences—part 2: bipolar disorders, schizophrenia-spectrum disorders, anxiety disorders, obsessive–compulsive disorders, trauma- and stressor-related disorders, personality disorders, substance-related and addictive disorders, neurocognitive disorders". European Archives of Psychiatry and Clinical Neuroscience. 265 (2): 87–106. doi:10.1007/s00406-014-0521-9. PMID 25155875.
- "The ICD-10 Classification of Mental and Behavioural Disorders" (PDF). WHO.
- International Classification of Diseases) ICD-10
- DeBoer LB, Powers MB, Utschig AC, Otto MW, Smits JA (August 2012). "Exploring exercise as an avenue for the treatment of anxiety disorders". Expert Review of Neurotherapeutics. 12 (8): 1011–22. doi:10.1586/ern.12.73. PMC 3501262. PMID 23002943.
- Barrientos, Ruth M.; Shukitt-Hale, Barbara; Layé, Sophie; Korosi, Aniko; Spencer, Sarah J. (2017-12-06). "Food for thought: how nutrition impacts cognition and emotion". NPJ Science of Food. 1 (1): 7. doi:10.1038/s41538-017-0008-y. ISSN 2396-8370. PMC 6550267. PMID 31304249.
- Dinsmoor, Robert Scott; Odle, Teresa G. (2015). "Generalized Anxiety Disorder". The Gale Encyclopedia of Medicine. 4 (5): 2149–2150.
- Bruce, M. S.; Lader, M. (2009). "Caffeine abstention in the management of anxiety disorders". Psychological Medicine. 19 (1): 211–4. doi:10.1017/S003329170001117X. PMID 2727208.
- Morissette, SB; Tull, MT; Gulliver, SB; Kamholz, BW; Zimering, RT (March 2007). "Anxiety, anxiety disorders, tobacco use, and nicotine: a critical review of interrelationships". Psychological Bulletin. 133 (2): 245–72. doi:10.1037/0033-2909.133.2.245. PMID 17338599.
- Rickels, K; Schweizer, E (1990). "The clinical course and long-term management of generalized anxiety disorder". Journal of Clinical Psychopharmacology. 10 (3 Suppl): 101S–110S. doi:10.1097/00004714-199006001-00017. PMID 1973934.
- Gould, Robert A.; Otto, Michael W.; Pollack, Mark H.; Yap, Liang (1997). "Cognitive behavioral and pharmacological treatment of generalized anxiety disorder: A preliminary meta-analysis". Behavior Therapy. 28 (2): 285–305. doi:10.1016/S0005-7894(97)80048-2.
- Bandelow, Borwin; Sher, Leo; Bunevicius, Robertas; Hollander, Eric; Kasper, Siegfried; Zohar, Joseph; Möller, Hans-Jürgen (June 2012). "Guidelines for the pharmacological treatment of anxiety disorders, obsessive–compulsive disorder and posttraumatic stress disorder in primary care" (PDF). International Journal of Psychiatry in Clinical Practice. 16 (2): 77–84. doi:10.3109/13651501.2012.667114. PMID 22540422. Retrieved 24 November 2015.
- Boschloo, L (2014). "The impact of lifestyle factors on the 2-year course of depressive and/or anxiety disorders". Journal of Affective Disorders. 159: 73–9. doi:10.1016/j.jad.2014.01.019. PMID 24679393.
- Behar, Evelyn; Dimarco, Ilyse Dobrow; Hekler, Eric B.; Mohlman, Jan; Staples, Alison M. (2009). "Current theoretical models of generalized anxiety disorder (GAD): Conceptual review and treatment implications". Journal of Anxiety Disorders. 23 (8): 1011–23. doi:10.1016/j.janxdis.2009.07.006. PMID 19700258.
- Ruiz, F. J. (2010). "A review of Acceptance and Commitment Therapy (ACT) empirical evidence: Correlational, experimental psychopathology, component and outcome studies". International Journal of Psychology and Psychological Therapy. 10 (1): 125–62.
- Hoyer, Jürgen; van der Heiden, Colin; Portman, Michael E. (February 2011). "Psychotherapy for Generalized Anxiety Disorder". Psychiatric Annals. 41 (2): 87–94. doi:10.3928/00485713-20110203-07.
- Cuijpers, Pim; Sijbrandij, Marit; Koole, Sander; Huibers, Marcus; Berking, Matthias; Andersson, Gerhard (2014-03-01). "Psychological treatment of generalized anxiety disorder: A meta-analysis". Clinical Psychology Review. 34 (2): 130–140. doi:10.1016/j.cpr.2014.01.002. ISSN 0272-7358. PMID 24487344.
- Barlow, D. H.: (2007) Clinical Handbook of Psychological Disorders, 4th ed.
- "A Guide to Understanding Cognitive and Behavioural Psychotherapies" Archived 2007-05-05 at the Wayback Machine, British Association for Behavioural and Cognitive Psychotherapies. Accessed 29 May 2007.
- "Generalized anxiety disorder", Mayo Clinic. Accessed 29 May 2007.
- Comer, Ronald (2014). Abnormal Psychology. New York, NY: Worth Publishers. pp. 114–122. ISBN 978-1-4641-3719-8.
- Roemer, Lizabeth; Orsillo, Susan M. (2006). "Expanding Our Conceptualization of and Treatment for Generalized Anxiety Disorder: Integrating Mindfulness/Acceptance-Based Approaches with Existing Cognitive-Behavioral Models". Clinical Psychology: Science and Practice. 9: 54–68. doi:10.1093/clipsy.9.1.54.
- Smout, M (2012). "Acceptance and commitment therapy - pathways for general practitioners". Australian Family Physician. 41 (9): 672–6. PMID 22962641.
- Baldwin, DS; Allgulander, C; Bandelow, B; Ferre, F; Pallanti, S (October 2012). "An international survey of reported prescribing practice in the treatment of patients with generalised anxiety disorder". The World Journal of Biological Psychiatry. 13 (7): 510–6. doi:10.3109/15622975.2011.624548. PMID 22059936.
- Carrasco, J. L.; Sandner, C. (December 2005). "Clinical effects of pharmacological variations in selective serotonin reuptake inhibitors: an overview". International Journal of Clinical Practice. 59 (12): 1428–1434. doi:10.1111/j.1368-5031.2005.00681.x. ISSN 1368-5031. PMID 16351675.
- Bech P, Lönn SL, Overø KF (2010). "Relapse prevention and residual symptoms: a closer analysis of placebo-controlled continuation studies with escitalopram in major depressive disorder, generalized anxiety disorder, social anxiety disorder, and obsessive-compulsive disorder". Journal of Clinical Psychiatry. 71 (2): 121–9. doi:10.4088/JCP.08m04749blu. PMID 19961809.
- Wagstaff, Antona J.; Cheer, Susan M.; Matheson, Anna J.; Ormrod, Douglas; Goa, Karen L. (2002-01-01). "Paroxetine: an update of its use in psychiatric disorders in adults". Drugs. 62 (4): 655–703. doi:10.2165/00003495-200262040-00010. ISSN 0012-6667. PMID 11893234.
- "Generalised anxiety disorder and panic disorder in adults: management | Guidance and guidelines | NICE". www.nice.org.uk. Retrieved 2018-11-02.
- "Antidepressant Medications for Children and Adolescents: Information for Parents and Caregivers". National Institute of Mental Health. Archived from the original on 1 March 2010. Retrieved 1 September 2015.
- Ferguson, James M. (February 2001). "SSRI Antidepressant Medications: Adverse Effects and Tolerability". Primary Care Companion to the Journal of Clinical Psychiatry. 3 (1): 22–27. doi:10.4088/PCC.v03n0105. ISSN 1523-5998. PMC 181155. PMID 15014625.
- Baldwin DS, Anderson IM, Nutt DJ, Allgulander C, Bandelow B, den Boer JA, Christmas DM, Davies S, Fineberg N, Lidbetter N, Malizia A, McCrone P, Nabarro D, O'Neill C, Scott J, van der Wee N, Wittchen HU (May 2014). "Evidence-based pharmacological treatment of anxiety disorders, post-traumatic stress disorder and obsessive-compulsive disorder: a revision of the 2005 guidelines from the British Association for Psychopharmacology". Journal of Psychopharmacology. 28 (5): 403–39. doi:10.1177/0269881114525674. PMID 24713617.
- Sansone RA, Sansone LA (March 2014). "Serotonin norepinephrine reuptake inhibitors: a pharmacological comparison". Innovations in Clinical Neuroscience. 11 (3–4): 37–42. PMC 4008300. PMID 24800132.
- Strawn, Jeffrey R.; Geracioti, Laura; Rajdev, Neil; Clemenza, Kelly; Levine, Amir (July 2018). "Pharmacotherapy for generalized anxiety disorder in adult and pediatric patients: an evidence-based treatment review". Expert Opinion on Pharmacotherapy. 19 (10): 1057–1070. doi:10.1080/14656566.2018.1491966. ISSN 1744-7666. PMC 6340395. PMID 30056792.
- Baldwin, David S; Anderson, Ian M; Nutt, David J; Allgulander, Christer; Bandelow, Borwin; den Boer, Johan A; Christmas, David M; Davies, Simon; Fineberg, Naomi (2014-04-08). "Evidence-based pharmacological treatment of anxiety disorders, post-traumatic stress disorder and obsessive-compulsive disorder: A revision of the 2005 guidelines from the British Association for Psychopharmacology" (PDF). Journal of Psychopharmacology. 28 (5): 403–439. doi:10.1177/0269881114525674. ISSN 0269-8811. PMID 24713617.
- Baldwin, David; Woods, Robert; Lawson, Richard; Taylor, David (2011-03-11). "Efficacy of drug treatments for generalised anxiety disorder: systematic review and meta-analysis". BMJ. 342: d1199. doi:10.1136/bmj.d1199. ISSN 0959-8138. PMID 21398351.
- Baldwin, David S.; Allgulander, Christer; Bandelow, Borwin; Ferre, Francisco; Pallanti, Stefano (October 2012). "An international survey of reported prescribing practice in the treatment of patients with generalised anxiety disorder". The World Journal of Biological Psychiatry. 13 (7): 510–516. doi:10.3109/15622975.2011.624548. ISSN 1814-1412. PMID 22059936.
- Baldwin, David S; Anderson, Ian M; Nutt, David J; Allgulander, Christer; Bandelow, Borwin; den Boer, Johan A; Christmas, David M; Davies, Simon; Fineberg, Naomi (2014-04-08). "Evidence-based pharmacological treatment of anxiety disorders, post-traumatic stress disorder and obsessive-compulsive disorder: A revision of the 2005 guidelines from the British Association for Psychopharmacology" (PDF). Journal of Psychopharmacology. 28 (5): 403–439. doi:10.1177/0269881114525674. ISSN 0269-8811. PMID 24713617.
- Katzman, Martin A.; Bleau, Pierre; Blier, Pierre; Chokka, Pratap; Kjernisted, Kevin; Van Ameringen, Michael; Canadian Anxiety Guidelines Initiative Group on behalf of the Anxiety Disorders Association of Canada/Association Canadienne des troubles anxieux and McGill University; Antony, Martin M.; Bouchard, Stéphane (2014). "Canadian clinical practice guidelines for the management of anxiety, posttraumatic stress and obsessive-compulsive disorders". BMC Psychiatry. 14 Suppl 1: S1. doi:10.1186/1471-244X-14-S1-S1. ISSN 1471-244X. PMC 4120194. PMID 25081580.
- Baldwin, David S; Anderson, Ian M; Nutt, David J; Allgulander, Christer; Bandelow, Borwin; den Boer, Johan A; Christmas, David M; Davies, Simon; Fineberg, Naomi (2014-04-08). "Evidence-based pharmacological treatment of anxiety disorders, post-traumatic stress disorder and obsessive-compulsive disorder: A revision of the 2005 guidelines from the British Association for Psychopharmacology" (PDF). Journal of Psychopharmacology. 28 (5): 403–439. doi:10.1177/0269881114525674. ISSN 0269-8811. PMID 24713617.
- Schueler, Y.-B.; Koesters, M.; Wieseler, B.; Grouven, U.; Kromp, M.; Kerekes, M. F.; Kreis, J.; Kaiser, T.; Becker, T. (April 2011). "A systematic review of duloxetine and venlafaxine in major depression, including unpublished data". Acta Psychiatrica Scandinavica. 123 (4): 247–265. doi:10.1111/j.1600-0447.2010.01599.x. ISSN 1600-0447. PMID 20831742.
- Cipriani, Andrea; Purgato, Marianna; Furukawa, Toshi A.; Trespidi, Carlotta; Imperadore, Giuseppe; Signoretti, Alessandra; Churchill, Rachel; Watanabe, Norio; Barbui, Corrado (2012-07-11). "Citalopram versus other anti-depressive agents for depression". The Cochrane Database of Systematic Reviews (7): CD006534. doi:10.1002/14651858.CD006534.pub2. ISSN 1469-493X. PMC 4204633. PMID 22786497.
- Chow, Robert M.; Issa, Mohammed (2017), "Serotonin-Norepinephrine Reuptake Inhibitors", Pain Medicine, Springer International Publishing, pp. 169–170, doi:10.1007/978-3-319-43133-8_44, ISBN 9783319431314
- Santarsieri, Daniel; Schwartz, Thomas L. (2015). "Antidepressant efficacy and side-effect burden: a quick guide for clinicians". Drugs in Context. 4: 212290. doi:10.7573/dic.212290. ISSN 1745-1981. PMC 4630974. PMID 26576188.
- Baldwin, David S.; Anderson, Ian M.; Nutt, David J.; Allgulander, Christer; Bandelow, Borwin; den Boer, Johan A.; Christmas, David M.; Davies, Simon; Fineberg, Naomi (May 2014). "Evidence-based pharmacological treatment of anxiety disorders, post-traumatic stress disorder and obsessive-compulsive disorder: a revision of the 2005 guidelines from the British Association for Psychopharmacology" (PDF). Journal of Psychopharmacology (Oxford, England). 28 (5): 403–439. doi:10.1177/0269881114525674. ISSN 1461-7285. PMID 24713617.
- Baldwin, David S; Anderson, Ian M; Nutt, David J; Allgulander, Christer; Bandelow, Borwin; den Boer, Johan A; Christmas, David M; Davies, Simon; Fineberg, Naomi (2014-04-08). "Evidence-based pharmacological treatment of anxiety disorders, post-traumatic stress disorder and obsessive-compulsive disorder: A revision of the 2005 guidelines from the British Association for Psychopharmacology" (PDF). Journal of Psychopharmacology. 28 (5): 403–439. doi:10.1177/0269881114525674. ISSN 0269-8811. PMID 24713617.
- Jurek, L.; Nourredine, M.; Megarbane, B.; d'Amato, T.; Dorey, J.-M.; Rolland, B. (2018-09-19). "[The serotonin syndrome: An updated literature review]". La Revue de Medecine Interne. 40 (2): 98–104. doi:10.1016/j.revmed.2018.08.010. ISSN 1768-3122. PMID 30243558.
- Bitter, Istvan; Filipovits, Dora; Czobor, Pal (November 2011). "Adverse reactions to duloxetine in depression". Expert Opinion on Drug Safety. 10 (6): 839–850. doi:10.1517/14740338.2011.582037. ISSN 1744-764X. PMID 21545241.
- Barlow, D. H., & Durand, V. M. (2009). Abnormal Psychology: An Integrative Approach. 5th Edition. Belmont: Wadsworth Cengage Learning.
- Durham, Rob C. (2007). "Treatment of generalized anxiety disorder". Psychiatry. 6 (5): 183–187. doi:10.1016/j.mppsy.2007.03.003.
- Allgulander, C; Bandelow, B; Hollander, E; Montgomery, SA; Nutt, DJ; Okasha, A; Pollack, MH; Stein, DJ; Swinson, RP; World Council Of, Anxiety (2003). "WCA recommendations for the long-term treatment of generalized anxiety disorder". CNS Spectrums. 8 (8 Suppl 1): 53–61. doi:10.1017/S1092852900006945. PMID 14767398.
- Stewart, S.; Westra, H. (2002). "Introduction to the Special Issue on: Benzodiazepine Side-Effects: From the Bench to the Clinic". Current Pharmaceutical Design. 8 (1): 1–3. doi:10.2174/1381612023396708. PMID 11812246.
- Bandelow, Borwin; Wedekind, Dirk; Leon, Teresa (2007). "Pregabalin for the treatment of generalized anxiety disorder: A novel pharmacologic intervention". Expert Review of Neurotherapeutics. 7 (7): 769–81. doi:10.1586/14737175.7.7.769. PMID 17610384.
- Owen, R. T. (2007). "Pregabalin: Its efficacy, safety and tolerability profile in generalized anxiety". Drugs of Today. 43 (9): 601–10. doi:10.1358/dot.2007.43.9.1133188. PMID 17940637.
- Wensel, T. M.; Powe, K. W.; Cates, M. E. (2012). "Pregabalin for the Treatment of Generalized Anxiety Disorder". Annals of Pharmacotherapy. 46 (3): 424–9. doi:10.1345/aph.1Q405. PMID 22395254.
- Rif S. El-Mallakh; S. Nassir Ghaemi (2 April 2007). Bipolar Depression: A Comprehensive Guide. American Psychiatric Pub. p. 158. ISBN 978-1-58562-651-9.
- Stephen M. Stahl; Bret A. Moore (13 February 2013). Anxiety Disorders: A Guide for Integrating Psychopharmacology and Psychotherapy. Routledge. p. 65. ISBN 978-1-136-44588-0.
- D. John Reynolds; Jamie Coleman; Jeffrey Aronson (10 November 2011). Oxford Handbook of Practical Drug Therapy. Oxford University Press. p. 765. ISBN 978-0-19-956285-5.
- "Generalised anxiety disorder and panic disorder in adults: management". National Institute of Health and Care Excellence. Retrieved 2 November 2018.
- Moffitt, Terrie E.; Harrington, H; Caspi, A; Kim-Cohen, J; Goldberg, D; Gregory, AM; Poulton, R (2007). "Depression and Generalized Anxiety Disorder". Archives of General Psychiatry. 64 (6): 651–60. doi:10.1001/archpsyc.64.6.651. PMID 17548747.
- Wolitzky-Taylor, Kate B.; Castriotta, Natalie; Lenze, Eric J.; Stanley, Melinda A.; Craske, Michelle G. (2010). "Anxiety disorders in older adults: A comprehensive review". Depression and Anxiety. 27 (2): 190–211. doi:10.1002/da.20653. PMID 20099273.
- Crocq, Marc-Antoine (June 1, 2017). "The History of Generalized Anxiety Disorder as a Diagnostic Category". Dialogues in Clinical Neuroscience. 19 (2): 107–116. PMC 5573555. PMID 28867935.
- Scott, E. L. (2011, September 6). Anxiety Disorders With Comorbid Substance Abuse. Psychiatric Times. Retrieved July 1, 2013, from http://www.psychiatrictimes.com/anxiety/anxiety-disorders-comorbid-substance-abuse
- Smith, Joshua P.; Book, Sarah W. (2010). "Comorbidity of generalized anxiety disorder and alcohol use disorders among individuals seeking outpatient substance abuse treatment". Addictive Behaviors. 35 (1): 42–5. doi:10.1016/j.addbeh.2009.07.002. PMC 2763929. PMID 19733441.
- Lee, S.; Wu, J.; Ma, Y. L.; Tsang, A.; Guo, W.-J.; Sung, J. (2009). "Irritable bowel syndrome is strongly associated with generalized anxiety disorder: A community study". Alimentary Pharmacology & Therapeutics. 30 (6): 643–651. doi:10.1111/j.1365-2036.2009.04074.x. PMID 19552631.
- "EBSCO Publishing Service Selection Page".
- "Access". Medscape. Retrieved 2013-01-15.
- Back SE, Brady KT (November 2008). "Anxiety Disorders with Comorbid Substance Use Disorders: Diagnostic and Treatment Considerations". Psychiatric Annals. 38 (11): 724–729. doi:10.3928/00485713-20081101-01. PMC 2921723. PMID 20717489.
- Shalev, I; Moffitt, Terrie Edith; Braithwaite, A W; Danese, A; Fleming, N I; Goldman-Mellor, S; Harrington, H L; Houts, R M; Israel, S; Poulton, R; Robertson, S P; Sugden, K; Williams, B; Caspi, A; et al. (2014-01-14). "Internalizing disorders and leukocyte telomere erosion: a prospective study of depression, generalized anxiety disorder and post-traumatic stress disorder" (PDF). Molecular Psychiatry. 19 (11): 1163–1170. doi:10.1038/mp.2013.183. PMC 4098012. PMID 24419039. Retrieved 21 April 2014.
- Kessler, Ronald C.; Keller, Martin B.; Wittchen, Hans-Ulrich (1 March 2001). "The Epidemiology of Generalized Anxiety Disorder". Psychiatric Clinics of North America. 24 (1): 19–39. doi:10.1016/S0193-953X(05)70204-5. PMID 11225507.
- Craighead, W. Edward (2013). Psychopathology: History, Diagnosis, and Empirical Foundations. John Wiley & Sons, Inc.
- Breslau, Naomi; Davis, Glenn C. (July 1985). "DSM-III generalized anxiety disorder: An empirical investigation of more stringent criteria". Psychiatry Research. 15 (3): 231–238. doi:10.1016/0165-1781(85)90080-0. PMID 3875873.
- Wittchen, Hans-Ulrich; Kessler, Ronald C.; Zhao, Shanyang; Abelson, Jamie (March–April 1995). "Reliability and clinical validity of UM-CIDI DSM-III-R generalized anxiety disorder". Journal of Psychiatric Research. 29 (2): 95–110. doi:10.1016/0022-3956(94)00044-R. PMID 7666382.
- Schacter, Daniel L.; Gilbert, Daniel T.; Wegner, Daniel M. (2011). "Generalized Anxiety Disorders". Psychology (2nd ed.). New York: Worth, Incorporated. pp. 559–560.
- Ballenger, JC; Davidson, JR; Lecrubier, Y; Nutt, DJ; Borkovec, TD; Rickels, K; Stein, DJ; Wittchen, HU (2001). "Consensus statement on generalized anxiety disorder from the International Consensus Group on Depression and Anxiety". The Journal of Clinical Psychiatry. 62 Suppl 11: 53–8. PMID 11414552.
- "Statistics". Mental Health Foundation. Retrieved 2018-12-19.
- "Relating the burden of anxiety and depression to effectiveness of treatment", World Health Organization.
- Canada, Public Health Agency of; Canada, Public Health Agency of (2017-01-31). "The burden of generalized anxiety disorder in Canada - HPCDP: Volume 37-2, February 2017". aem. Retrieved 2018-12-19.
- "Anxiety Disorders: Background, Anatomy, Pathophysiology". 1 December 2016 – via eMedicine. Cite journal requires
|journal=(help) - Kessler, Ronald C.; Chiu, WT; Demler, O; Merikangas, KR; Walters, EE (2005). "Prevalence, Severity, and Comorbidity of 12-Month DSM-IV Disorders in the National Comorbidity Survey Replication". Archives of General Psychiatry. 62 (6): 617–27. doi:10.1001/archpsyc.62.6.617. PMC 2847357. PMID 15939839.
- Grant, Bridget F.; Hasin, Deborah S.; Stinson, Frederick S.; Dawson, Deborah A.; June Ruan, W.; Goldstein, Risë B.; Smith, Sharon M.; Saha, Tulshi D.; Huang, Boji (2005). "Prevalence, correlates, co-morbidity, and comparative disability of DSM-IV generalized anxiety disorder in the USA: Results from the National Epidemiologic Survey on Alcohol and Related Conditions". Psychological Medicine. 35 (12): 1747–59. doi:10.1017/S0033291705006069. PMID 16202187.
- Robins LN, Regier DA, eds. Psychiatric disorders in America: the Epidemiologic Catchment Area Study. New York: The Free Press, 1991.
- Albano, Anne Marie; Chorpita, Bruce F.; Barlow, David H. (2003). "Childhood Anxiety Disorders". In Mash, Eric J.; Barkley, Russell A. (eds.). Child Psychopathology (2nd ed.). New York: Guilford Press. pp. 279–329. ISBN 978-1-57230-609-7.
- Keeton, CP; Kolos, AC; Walkup, JT (2009). "Pediatric generalized anxiety disorder: epidemiology, diagnosis, and management". Paediatric Drugs. 11 (3): 171–83. doi:10.2165/00148581-200911030-00003. PMID 19445546.
Further reading
- Brown, T. A., O'Leary, T. A., & Barlow, D. H. (2001). "Generalised anxiety disorder". In D. H. Barlow (ed.), Clinical handbook of psychological disorders: A step-by-step treatment manual (3rd ed.). New York: Guilford Press.
- Barlow, D. H., & Durand, V. M. (2005). Abnormal psychology: An integrative approach. Australia; Belmont, Calif.: Wadsworth.
- Tyrer, Peter; Baldwin, David (2006). "Generalised anxiety disorder". The Lancet. 368 (9553): 2156–66. doi:10.1016/S0140-6736(06)69865-6. PMID 17174708.
External links
| Classification | |
|---|---|
| External resources |
|
- Mayo Clinic – Information on diagnosis and treatment for GAD
- WebMD – Information on symptoms and causes of GAD
- Anxiety Disorders Association of America – Information for families, clinicians, and researchers
- National Institute of Mental Health, Generalized Anxiety Disorder: When Worry Gets Out of Control
- National Center for Complementary and Integrative Health, Anxiety and Complementary Health Approaches